It’s an exciting time in the world of femtech with multiple products being developed for taking our overnight temperature.
Oura Ring is a new player in fertility awareness. Oura Ring partnered with Natural Cycles, a temperature-only (with optional LH) fertility awareness based method. As of 2022, the ring is approved for use with syncing with Natural Cycles.
As a traditional charter of my cycle, I wanted to see if Oura Ring would be a good fit as a cross-check to help confirm ovulation without syncing to Natural Cycles.
After five cycles of use and comparisons to other thermometers, I am confident in saying that Oura Ring can be used as sympto-thermal method cross check with some tweaking and conversions. Read on if you would like to see examples and my method of conversion in order to avoid paying that extra fee to Natural Cycles.
First and foremost, you should know that no wearable has current been studied for traditional fertility awareness sympto-thermal methods. Even Natural Cycles has only done a small study of 40 charters to prove that the ring is equivalent to old-school basal body temperature. They found that it mostly lined up, albeit that the Oura temperature often confirmed one day sooner.
If you are charting to avoid pregnancy and reading this article, I highly recommend cross-checking with cervical mucus, cervical position, and/or urinary hormones in addition to the Ring. I do NOT recommend using the Ring alone to avoid pregnancy. If you are seriously avoiding, you should use at least one of the signs mentioned above and wait until those rules are met before having unprotected sex. You should cross-check with oral or vaginal temperatures for a minimum of 2-3 cycles before relying on Oura to confirm ovulation.
We just don’t have the kind of evidence necessary for me to recommend using Oura without other fertility signs, particularly for those strictly avoiding a pregnancy. If you are charting to conceive, then this Ring is perfectly acceptable for confirming you are in your luteal phase.
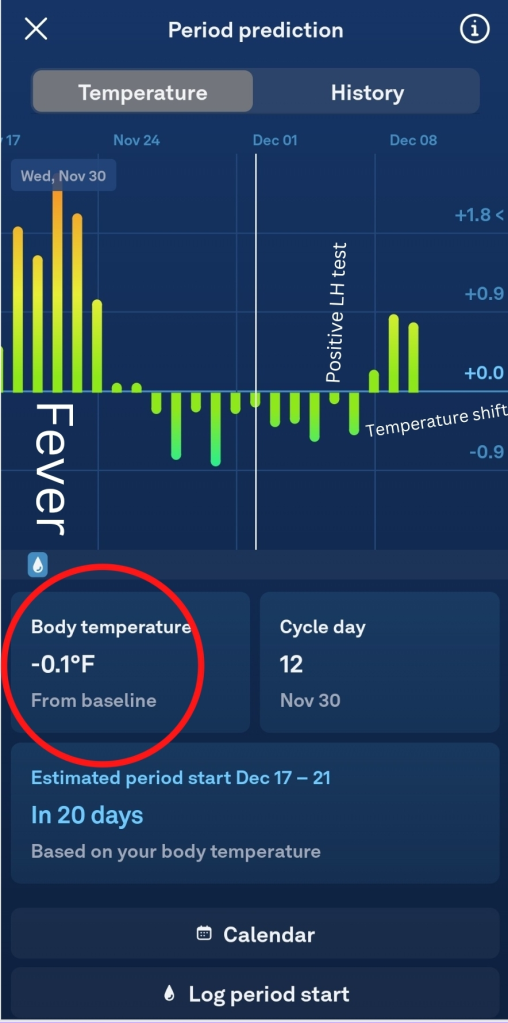
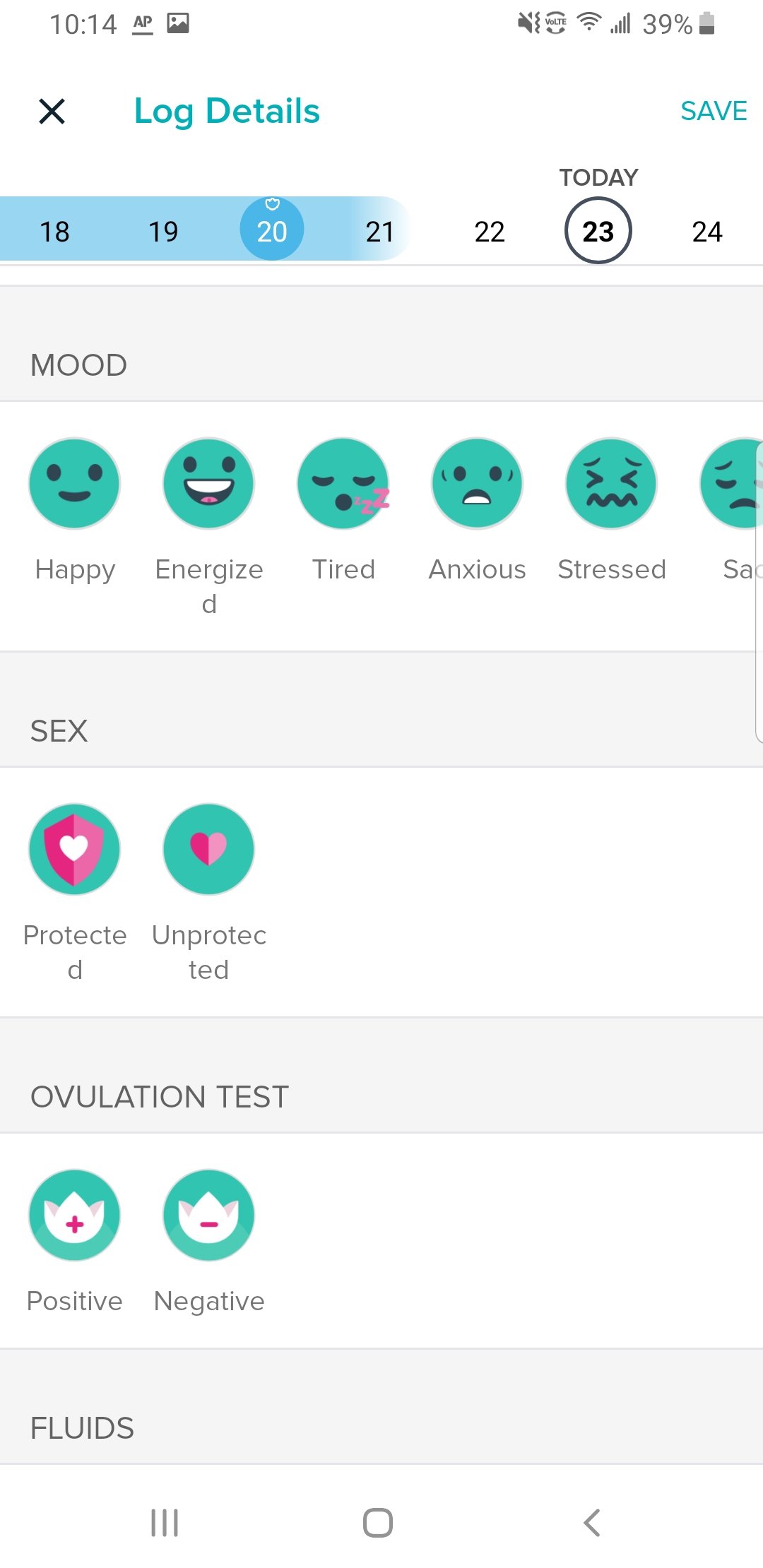
Oura Ring is worn 24/7 for full use of its features. Overnight, it detects your sleep and a temperature is determined at this time. Your temperature is displayed when you sync Oura to the app in the morning as a +/- deviation from baseline, as shown in the photo above.
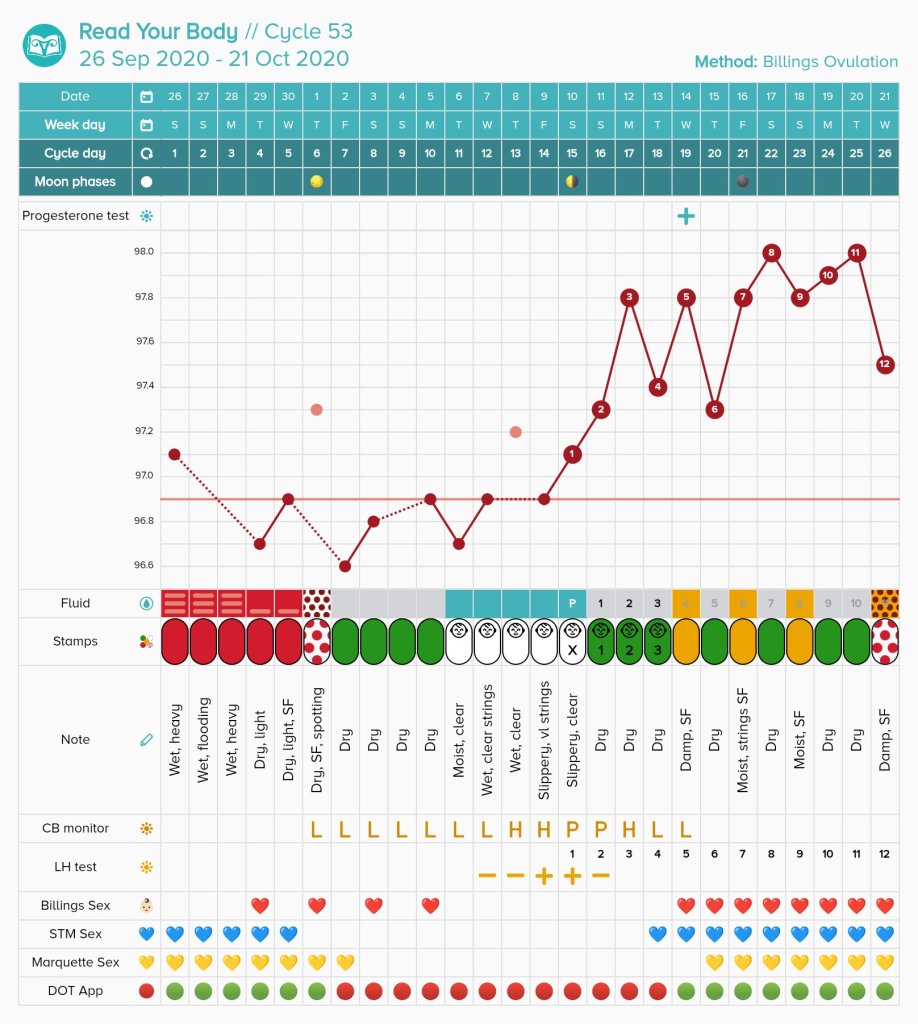
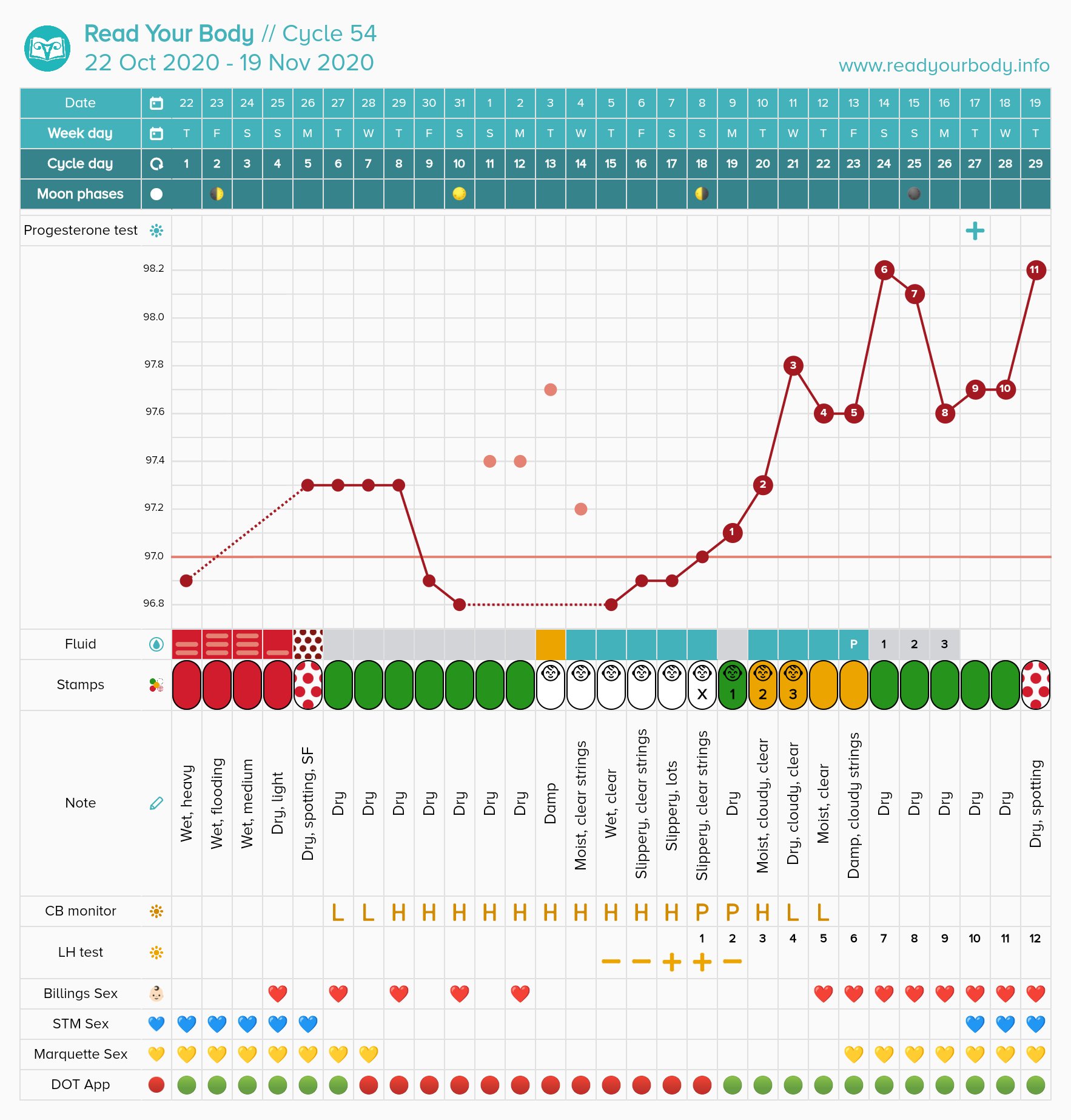
To chart your temperature in an app without Natural Cycles, you will need to choose a baseline. Remember, when we are charting our cycles, we are pattern making. You will need to translate the deviation to the chart so that you can see a pattern of lower and higher temperatures. I chose 97 degrees Fahrenheit as my baseline because it is a whole number that falls in the middle of most fertility awareness charts.

Traditional methods call for two decimal points. However, this isn’t necessary to see a pattern with ring temperature. Finger temperature tends to show larger temperature shifts than standard waking body temperature taken at the mouth.
If you want to see two decimal places, you must initially purchase a subscription with Natural Cycles.
The official statement from Oura is that you shouldn’t compare it to other thermometers or use it without Natural Cycles. The reason they say not to compare it is because all thermometers will give different results. As charters, we are smart enough to know that we are looking for patterns and not the exact same result. The reason that they say to use it with Natural Cycles is likely because of the paid partnership as well as to avoid liability for unintended pregnancies. I’d like to say again that using Oura for a traditional FAM without Natural Cycles only has case study level evidence and is not currently endorsed by any organizations. Consider this when choosing it!

What else does Oura ring do that can help me track my cycle health?
- Sleep information (quality, amount, phases, disturbance)
- Steps, exercise, calories
- Meditation and winding down for sleep
- Stress levels, illness
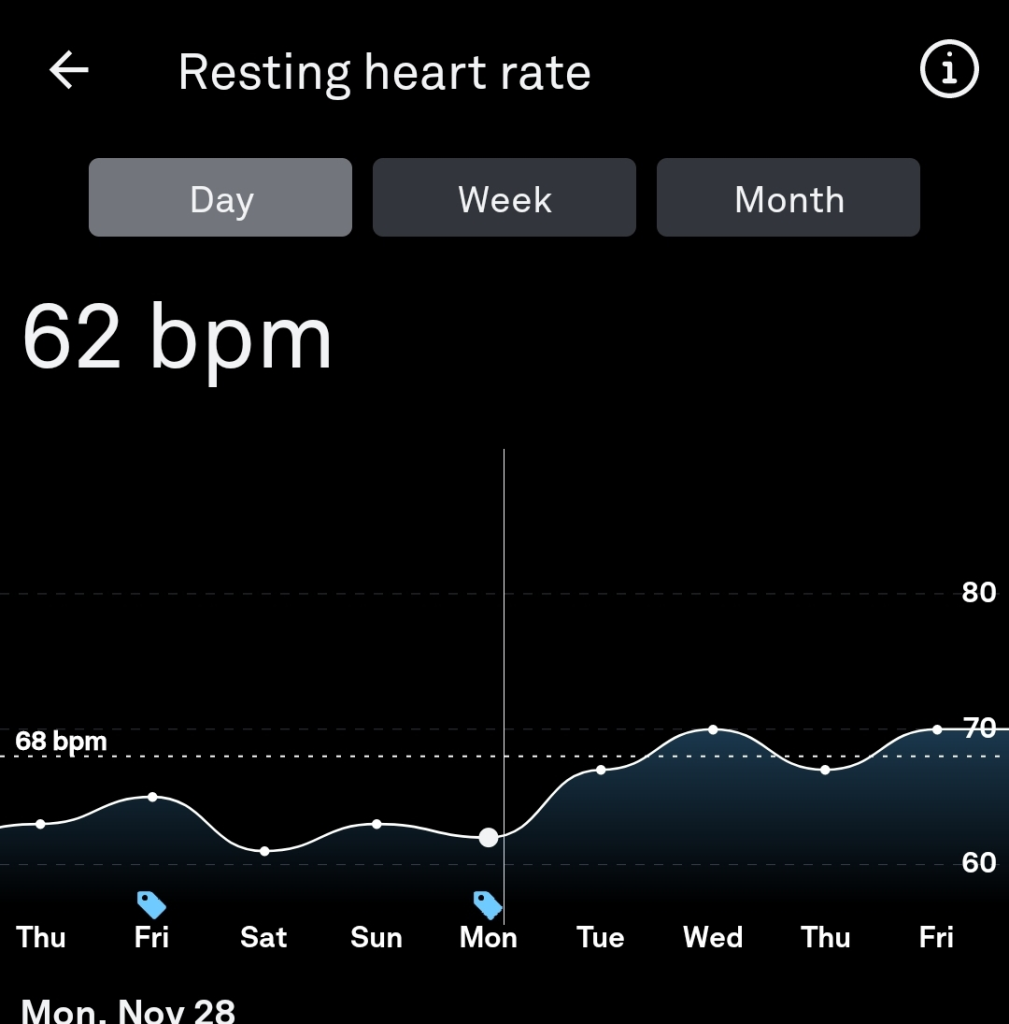
- Resting heart rate and sleeping heart rate
- Rest mode feature. If you have painful periods or are debilitated by any illness, Oura can be informed that you are sick or unwell and your statistics on it will change.
What are the details?
- It is initially approximately $300 USD depending on the model and time of year.
- It is free to the use the app for the first 6 months, and then it is $5.99 USD per month. I’ve heard some people say they have used without subscribing, but can’t say if temperature feature is available without paying.
- The battery life is about 5-7 days with all day use and takes about 30 minutes to fully charge.
You can use my link for $50 USD off. This link only works for five people. I will periodically replace the link once a new one becomes available.
For me, the greatest selling point for this ring is NEVER having to remember taking your temperature again. I’m an adult with a busy life and this makes charting so much easier for me. I charge my ring once a week and otherwise forget about it. This is definitely my current favorite femtech for charting your cycle.



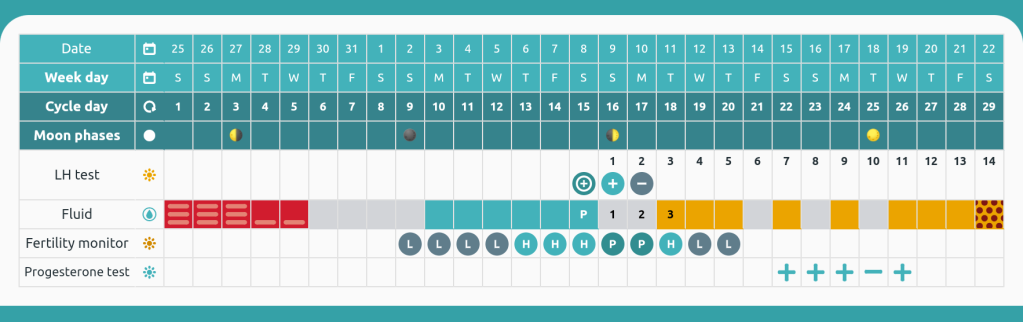

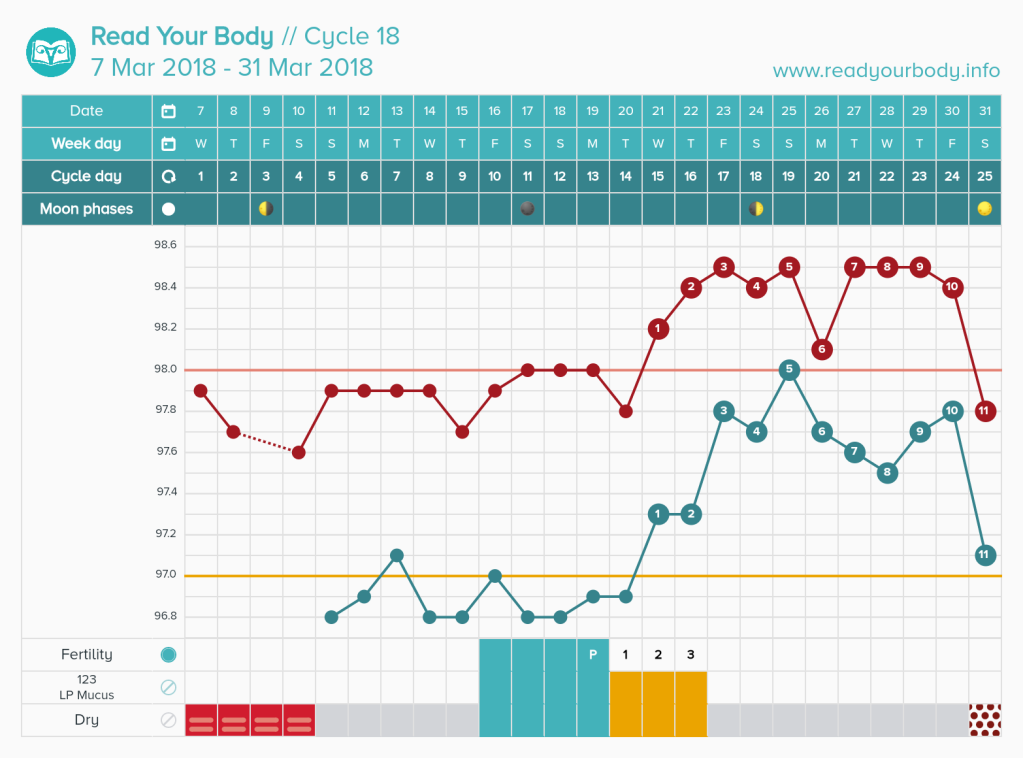




















You must be logged in to post a comment.